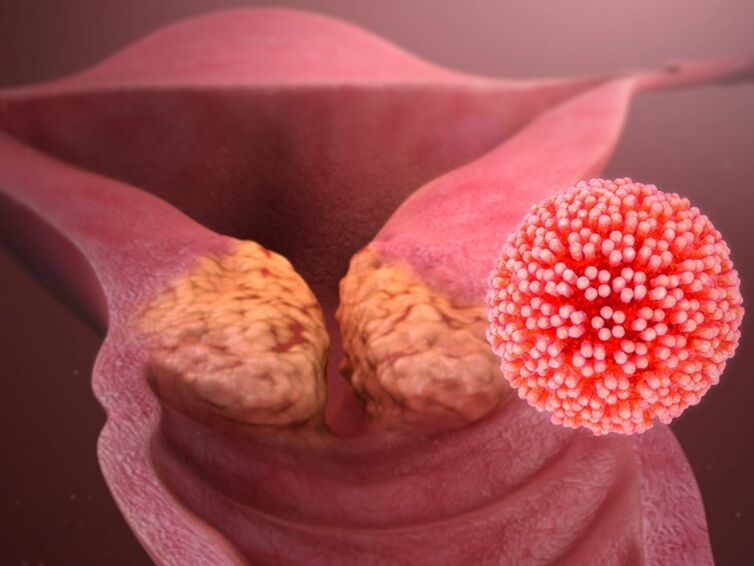
The human papillomavirus (HPV) provokes the formation of papillomas, warts, condylomas and is a triggering factor in the development of cancer of the cervix and laryngopharynx. Less commonly, it can affect the oral mucosa, esophagus, conjunctiva of the eyes. According to the World Health Organization, the incidence of this infection has increased 10 times over the past 10 years. In our country, the prevalence of HPV infection, according to studies in the regions, varies from 29% to 45%. The medical community is particularly wary due to the fact that about a third of all isolated virus genotypes provokes the development of oncological pathology.
Classification of the course of papillomavirus infection
Getting into the body of a woman, HPV can show different activity, which depends on the state of immunity. Depending on how the pathogen behaves, there are several variants of human papillomavirus infection:
- latent flow. The virus persists in the body, but does not cause pathological changes in the cells. There are no symptoms - the presence of a microorganism can only be determined using molecular biological research methods.
- HPV-associated inflammation As a rule, we are talking about cervicitis or vulvovaginitis on the background of HPV, which lead the patient to a gynecologist. In consultation, she can find out: how to treat HPV in women. It should be understood that the virus does not cause inflammation on its own, but creates conditions for the activation of the inflammatory process.
- Condylomas located in the anogenital region and on the mucous membrane of the genital tract are a form of the course of PVI (papillomavirus infection), in which it becomes necessary to use modern surgical techniques to remove formations. After surgical removal, laser destruction, cryodestruction or radio wave coagulation, complex treatment is required to prevent complications and relapses.
- Dysplasia of the cervix. May be asymptomatic or cause discharge. Severe forms of the disease are precancerous - in order to avoid this situation, a correct understanding of how HPV is treated in women is more important than ever.
Classification helps the doctor to choose the most effective treatment tactics. Pathogen strains are also divided into groups depending on the ability to cause oncological diseases: HPV with high, medium and low oncogenic risk. Among the 40 variants of the virus transmitted through sexual contact, 14 are classified as high and medium oncogenic risk: -16, -18, -31, -33, -35, -39, -45, -51, -52, -56, -58, -59, -66 and -68 types.
How is the human papillomavirus transmitted?
Among the female population, HPV infection reaches 70%. However, the presence of a pathogen in the body does not mean a disease. If a person has a healthy immune system, then HPV infection, in most cases, is transient in nature - it disappears on its own within 2 years. If this does not happen, the question of how to treat human papillomavirus in women becomes relevant.
The main route of transmission of the virus is contact:
- sexual;
- vertical (from mother to fetus during childbirth);
- household (when using one towel, razor, underwear).
Young people aged 13-30 are most susceptible to infection with the virus. At the first sexual contact, the risk of infection is about 60%. The virus can also enter the body in the absence of direct intercourse. It is girls who are most at risk of HPV, and then with its consequences. This is due to the peculiarities of the structure of their genital organs.
Human papillomavirus in women: causes
Among the female population, HPV infection reaches 70%. However, the presence of a pathogen in the body does not mean a disease. If a person has a healthy immune system, then HPV infection, in most cases, is transient in nature - it disappears on its own within 2 years. If this does not happen, the question of how to treat human papillomavirus in women becomes relevant.
- concomitant pathology of the reproductive system;
- endocrine disorders;
- immunodeficiencies and beriberi;
- frequent acute infectious diseases - SARS, other viral and bacterial infections;
- early sexual intercourse;
- abortions;
- smoking and drinking alcohol;
- chronic psycho-emotional stresses that weaken the immune system;
- excessive physical and emotional stress, irregular daily routine;
- postpartum period - due to stress and hormonal changes;
- long-term use of immunosuppressive drugs and oral contraceptives.
Frequent change of sexual partners also increases the risk of both infection with new strains of the virus and activation of an existing infection. If immunity is reduced, the virus is integrated into the cellular genome, which entails a high probability of cancer - how to cure HPV in women at this stage of medical science has yet to be discovered. Therefore, it is so important to keep the activity of the virus under control and properly stimulate the immune defense.
The first signs of HPV in women and additional symptoms
The most obvious sign of the presence of HPV in a woman's body is the appearance of papillomas on the mucous membranes of the genital organs and the skin of the anogenital region. They do not cause pain and, as a rule, go unnoticed for a long time. However, the activity of the virus can provoke the appearance of other unpleasant symptoms, due to which a woman will immediately contact a gynecologist:
- pathological discharge from the vagina, accompanied by itching and burning;
- frequent relapses of vaginitis, bacterial vaginosis;
- foul-smelling vaginal discharge.
On examination, the doctor sees benign formations on the skin, changes in the epithelium of the cervix, signs of inflammation. Cancer can appear only in the later stages of a chronic papillomavirus infection.
Is there a cure for human papillomavirus?
In order to understand how HPV is currently being treated in women, it is necessary to understand what approaches exist in the treatment of human papillomavirus infection. At the moment, HPV infection therapy is reduced to the following activities:
- prevention of the progression of HPV infection;
- elimination of clinical manifestations;
- stimulation of systemic and local antiviral immunity.
There are no drugs that lead to the complete disappearance of the virus from the body. However, research in this area is ongoing - the focus of doctors is focused on the need for combined treatment of various manifestations of HPV. Research in the field of genetic engineering is promising. Scientists are considering the possibility of "rewriting" the viral code to self-destruct instead of spreading. Reducing viral copies restores local immunity and eliminates chronic inflammation.
Information for doctors on the topic "HPV how to treat in women" is currently detailed in the current clinical guidelines.
When is it necessary to see a doctor?
Women should undergo a preventive examination by a gynecologist at least once a year. Also, the need to visit a doctor arises when any disturbing symptoms appear:
- neoplasms in the genital area;
- warts on other areas of the skin and mucous membranes;
- pain in the lower abdomen;
- unusual discharge or bad smell from the vagina;
- itching, swelling, redness of the genitals.
In a situation where an accidental sexual intercourse has occurred, it is recommended to visit a gynecologist. He will conduct an examination, take a gynecological smear and scraping to detect HPV.
If papillomas occur in other parts of the body, a consultation with a dermatovenereologist is necessary. When papillomas or condylomas grow in the anus, the intervention of a proctologist may be required. This will help determine the tactics of treatment and what remedies for papilloma should be prescribed to the patient in a particular case for purchase at a pharmacy.
General scheme of therapy
The primary weapon in the fight against HPV is the stable immunity of the person himself. The American Center for Disease Control and Prevention draws attention to the fact that in 90% of cases of contact with the virus, clinical manifestations do not develop due to self-suppression of the virus by natural immunity.
Treatment for HPV infection should be comprehensive and aimed at:
- therapy of concomitant diseases;
- elimination of external manifestations of diseases - medically and, if necessary, surgically;
- reduction in viral load;
- stimulation of the body's own defenses.
Chronic psycho-emotional stress, poor environment and comorbidities reduce the ability of a woman's immune system to cope with the virus on its own. There are drugs that, having a direct antiviral and immunomodulatory effect, help the body's strength and lead to a decrease in viral load. These modern drugs include a spray with activated glycyrrhizic acid, which is obtained from licorice root. It helps stop the virus from replicating early and reduces the number of copies of HPV genetic material in the body. The tool has a special intravaginal nozzle for drug delivery to the cervix and its uniform distribution along the walls of the vagina. Antiviral and immunomodulatory therapy in the latent course of papillomavirus infection can prevent the appearance of unpleasant symptoms and the transition of the infection to more aggressive forms. If the virus provoked changes in the genital area and cervical epithelium, the spray helps:
- relieve inflammation;
- eliminate itching;
- restore the integrity of the mucosa;
- increase local immunity.
The use of the product is also indicated in the period of preparation for the removal of benign formations caused by HPV, to reduce the activity of the virus and prevent relapses. The drug helps to regenerate the skin and prevent the attachment of a secondary infection.
Removal of papillomas and warts
Benign formations caused by HPV are subject to removal, which can be carried out by the following methods:
- cryodestruction - exposure to the neoplasm with cold;
- electrocoagulation - treatment with high frequency current;
- laser removal - layer-by-layer exposure to laser irradiation until a scab appears;
- chemical destruction - treatment with special chemical solutions that are applied to warts and destroy them;
- surgical removal - given the high risk of recurrence after this type of destruction, it is prescribed selectively - if it is impossible to use other methods.
Among the new developments in the treatment of HPV is the CRISPR / Cas9 system, which almost completely cuts the DNA and embeds its sections, thereby inactivating the further spread of the virus.
Prevention
For primary prevention, it is recommended to use barrier contraception (condoms), which, although not absolute protection against HPV, will reduce the level of exposure to the virus. You should be selective in your choice of sexual partners. If an accidental connection did take place, a special spray can be used to protect against HPV, herpes simplex virus and cytomegalovirus infection.
To date, HPV vaccination is the most effective. It protects against the most common and malignant types of human papillomavirus. In many countries, HPV vaccination is included in the mandatory immunization calendar. The most effective time for vaccination is in childhood and adolescence. Previously, it was believed that after 20 years of vaccination does not make sense. But recent studies have shown that HPV vaccination is appropriate and effective until the age of 45-47.
If a virus infection does occur, the task of secondary prevention is to maintain the good health of the patient, in particular the good condition of his immune system. Women should regularly visit a gynecologist to detect virus-associated diseases in the early stages.













































































